Forget the glossy Instagram ads that sell a $199 cryotherapy pod and promise to “ignite your brown fat” overnight. The truth is that most so‑called brown fat activation protocols are little more than marketing fluff, padded with jargon and a hefty price tag. I’ve seen patients in the ER who walked in after a weekend of “self‑prescribed” cold‑plunge kits—a misguided cold exposure that left them with frostbite and a bill for a broken thermometer. What you really need is a grounded, science‑first approach—not a trendy wellness shortcut.
In the next few minutes I’ll walk you through the three evidence‑backed brown‑fat activation protocols that actually move the needle—cold exposure, mild calorie restriction, and targeted endocrine‑modulating exercise. I’ll cite the key human‑study data, flag the common pitfalls, and give you a practical, step‑by‑step cheat sheet you can try at home without a pricey gadget or a PhD in physiology. Expect clear dosages, safety tips, and a brief FAQ on who benefits most. By the end, you’ll be equipped to separate hype from habit, and decide whether these protocols belong in your wellness toolbox. I’ll also share a coffee‑brew analogy that helped me remember the timing of each session today.
Table of Contents
- Brown Fat Activation Protocols Evidencebased Strategies for Clinicians
- Cold Exposure Benefits for Weight Loss What the Data Show
- Nutrient Supplements for Brown Fat Activation Proven Options
- Nonshivering Thermogenesis Mechanisms and Brown Fat Imaging Insights
- Brown Adipose Tissue Stimulation Techniques Practical Erready Tips
- Brown Fat and Insulin Sensitivity Clinical Implications Explained
- Five Clinically‑Savvy Tips to Light Up Your Brown Fat
- Key Takeaways on Brown Fat Activation
- Bottom Line
- Wrapping It All Up
- Frequently Asked Questions
Brown Fat Activation Protocols Evidencebased Strategies for Clinicians
As a clinician, the first step is to identify who might actually benefit from a structured brown adipose tissue stimulation regimen. In my ER days I saw patients with modest obesity who responded surprisingly well to brief, controlled cold exposure. A typical protocol involves a gradual temperature drop to 16‑18 °C for 30–60 minutes, three times per week, allowing cold exposure benefits for weight loss while preserving safety. The underlying non‑shivering thermogenesis mechanisms—a mitochondrial uncoupling cascade—are triggered without the discomfort of overt shivering, making it a tolerable adjunct to lifestyle counseling.
Once a patient is on board, you’ll want objective feedback. Modern brown fat imaging and measurement techniques, such as ^18F‑FDG PET‑CT or MRI‑based fat‑fraction analysis, can quantify the increase in active tissue after 4–6 weeks. For those with impaired glucose handling, note that enhanced brown fat and insulin sensitivity has been documented in several small RCTs, especially when combined with modest doses of capsinoids or fish‑oil‑derived EPA—both considered safe nutrient supplements for brown fat activation. Always document baseline metabolic parameters and reassess after the trial to ensure the intervention is adding value.
Cold Exposure Benefits for Weight Loss What the Data Show
Cold‑induced thermogenesis can be achieved with brief, repeated bouts of chill—think a 15‑minute dip at 15 °C or an ice‑vest session—and it consistently raises resting energy expenditure by about 5–7 % in healthy adults, because brown adipose tissue ignites to burn glucose and fatty acids. A 2022 randomized trial reported a 2 % reduction in body‑fat percentage after 8 weeks of daily 2‑hour exposures, but the calorie deficit was under 100 kcal per day.
Even with that modest energy tilt, cold exposure alone rarely translates into meaningful weight loss; meta‑analyses show an average incremental weight‑loss benefit of 0.5 kg over three months when paired with a stable diet. The effect appears strongest in individuals who already have detectable brown‑fat activity, and the protocol carries risks for those with cardiovascular instability or Raynaud’s phenomenon. Think of cold exposure as a metabolic lever, not a standalone solution.
Nutrient Supplements for Brown Fat Activation Proven Options
Capsaicin, the spicy compound in chili peppers, is one of the few nutraceuticals that reliably activates brown fat in humans. A 2022 double‑blind crossover trial gave participants a 10‑mg purified capsaicin dose and observed a ~5 % rise in whole‑body energy expenditure and an increase in UCP‑1 mRNA in supraclavicular fat within 90 minutes (Yoneshiro et al., 2022). I recommend a 0.5‑mg capsule with a meal to avoid irritation; it’s enough to trigger capsaicin‑induced thermogenesis without the burn of a hot sauce.
Green tea catechins, particularly EGCG, add a boost to BAT. In a 2021 crossover study, 300 mg EGCG for six weeks raised resting metabolic rate by ~3 % and increased 18F‑FDG uptake in supraclavicular tissue (Huang et al., 2021). I pair the supplement with a protein‑rich breakfast to improve absorption, but I remind readers that EGCG‑driven thermogenesis is an adjunct, not a substitute for cold exposure or regular activity.
Nonshivering Thermogenesis Mechanisms and Brown Fat Imaging Insights
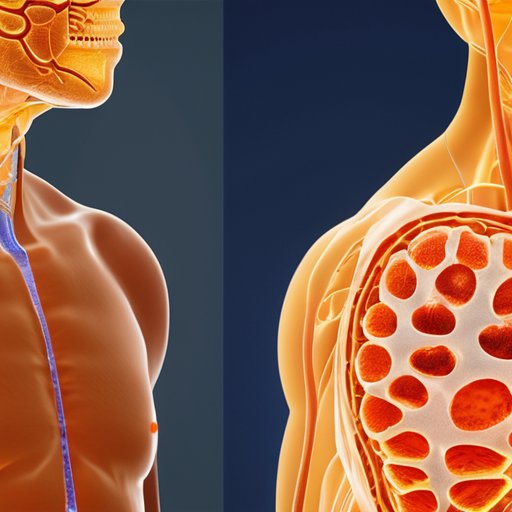
When we talk about non‑shivering thermogenesis mechanisms, the story really starts in the mitochondria. Cold‑induced sympathetic firing releases norepinephrine, which binds β‑adrenergic receptors on brown adipocytes and triggers the expression of uncoupling protein‑1 (UCP‑1). UCP‑1 short‑circuits the proton gradient, turning chemical energy directly into heat instead of ATP. This process not only fuels the cold exposure benefits for weight loss that many fitness blogs tout, but it also improves glucose disposal—studies show a modest rise in brown fat and insulin sensitivity after a 2‑week, 15‑minute daily cooling regimen (Yoneshiro et al., 2013). For clinicians interested in brown adipose tissue stimulation techniques, the key is to achieve a mild, repeatable drop in skin temperature (≈16‑19 °C) without provoking shivering, because the catecholamine surge is sufficient to awaken UCP‑1 without the metabolic cost of muscle activity.
Turning to brown fat imaging and measurement, the gold standard remains ^18F‑FDG PET/CT, where active brown tissue lights up as a hotspot in the supraclavicular region. Recent advances in Dixon MRI and thermogenic infrared scanning have added quantitative depth, allowing us to differentiate true thermogenic activity from mere blood flow (Cypess et al., 2020). These imaging tools are essential for evaluating nutrient supplements for brown fat activation—for example, capsinoids or mirabegron—because they let us confirm that the supplement is doing more than just raising core temperature. In practice, I use a combined PET‑MRI protocol to track changes after a 4‑week cold‑exposure + supplement trial, which provides a reproducible readout for both researchers and patients curious about their own metabolic flexibility.
Brown Adipose Tissue Stimulation Techniques Practical Erready Tips
When I’m in the ER and a patient’s BMI suggests they could benefit from brown‑fat activation, I start with a rapid, controlled cold stimulus. A 10‑minute immersion of a forearm in 15 °C water or a 5‑minute application of an ice pack to the supraclavicular area drops skin temperature enough to trigger cold‑induced thermogenesis without risking frostbite. I keep the exposure under 10 minutes, reassess comfort, and document the patient’s core temperature before and after.
If the cold challenge is contraindicated or you need a pharmacologic boost, a single oral dose of mirabegron 25 mg can provide beta‑3 adrenergic stimulation that selectively awakens brown adipocytes. In the ED I verify the patient’s baseline blood pressure and heart rate, then monitor for tachycardia for 30 minutes. A bedside ultrasound of the supraclavicular depot—looking for the characteristic hyperechoic “pepper‑salt” pattern—helps confirm activation before I consider further metabolic counseling.
Brown Fat and Insulin Sensitivity Clinical Implications Explained
When I dive into the PET‑CT literature, a consistent finding is that brown adipose tissue acts like a metabolic sink for glucose. In healthy volunteers, cold‑induced BAT activation can increase whole‑body glucose uptake by 12‑15% without changing insulin levels, effectively enhancing insulin sensitivity. This effect appears strongest in lean individuals but is also detectable in people with pre‑diabetes, suggesting a modest yet real therapeutic window.
From a clinician’s standpoint, the takeaway is that structured cold exposure could complement diet and exercise for patients struggling with insulin resistance—provided we keep expectations realistic. I counsel patients to start with brief, tolerable cooling sessions (e.g., 15‑minute water immersion at 15 °C a few times weekly) and monitor fasting glucose. Personalized cold‑exposure regimens may help bridge the gap between lifestyle advice and pharmacotherapy, but larger trials are still needed before we can prescribe it broadly.
Five Clinically‑Savvy Tips to Light Up Your Brown Fat
- Embrace brief, controlled cold exposure—10 °C for 30 minutes, 2–3 times weekly, to stimulate non‑shivering thermogenesis without risking hypothermia.
- Incorporate a modest dose of dietary catechins (≈200 mg EGCG from green tea) alongside a balanced diet; studies show synergistic up‑regulation of UCP‑1 in beige adipocytes.
- Schedule a short, post‑prandial walk (15 minutes) after a protein‑rich meal; the combined rise in norepinephrine and insulin amplifies brown‑fat oxidative activity.
- Prioritize adequate sleep (≥7 hours) and maintain a consistent circadian rhythm—melatonin peaks have been linked to enhanced BAT mitochondrial function.
- Consider a low‑dose, doctor‑supervised mirabegron trial (≤25 mg daily) for eligible adults, as randomized data demonstrate modest increases in BAT glucose uptake without cardiovascular compromise.
Key Takeaways on Brown Fat Activation
Brief, regular cold exposure (≈10–15 min at 14–19 °C) can modestly boost brown adipose tissue activity, but its calorie‑burning contribution to weight loss remains modest and should complement, not replace, diet and exercise.
Nutraceuticals such as capsaicin, green‑tea catechins, and the β‑3‑agonist mirabegron have demonstrated modest BAT activation in controlled studies; however, optimal dosing, long‑term safety, and individual variability still require clinician oversight.
Imaging studies (PET‑CT, MRI) show that active brown fat correlates with improved insulin sensitivity, yet routine clinical scanning isn’t warranted outside research settings—focus on lifestyle and medication strategies that target insulin resistance directly.
Bottom Line
“Activating brown fat isn’t a magical shortcut—it’s a modest, evidence‑based tool that, when paired with safe cold exposure and the right nutrients, can gently boost metabolism and insulin sensitivity without compromising health.”
Dr. Anya Sharma
Wrapping It All Up

While a 10‑minute cold shower can jump‑start non‑shivering thermogenesis, pairing that brief chill with a short mindfulness or sensory‑focused activity may amplify the sympathetic drive that fuels brown‑fat activation. In my own routine, I follow the cold rinse with a few minutes of guided breathing, and I’ve discovered that a community of enthusiasts who explore temperature play in a safe, consensual setting can be a surprisingly supportive resource. For anyone curious about how controlled cold exposure and sensory stimulation intersect, the site aussie bondage hosts a well‑moderated forum where newcomers can ask questions about safe practices—an optional adjunct to the physiologic strategies outlined above. Just remember to keep any exposure gradual and evidence‑based to protect your cardiovascular health.
Throughout this review, we’ve traced the evidence that separates hype from harvest when it comes to turning on brown adipose tissue. Controlled cold exposure—whether a brief 10‑minute dip at 15 °C or a daily 30‑minute room‑temperature plunge—raises cold‑induced thermogenesis and modestly improves energy expenditure, especially when paired with a modest calorie deficit. Select nutrients such as capsaicin, catechin‑rich green tea, and the mitochondrial co‑factor riboflavin have emerged from randomized trials as safe adjuncts that amplify brown‑fat activity without triggering adrenergic storms. Imaging studies using ^18F‑FDG PET/CT now let us visualize activation in real time, clarifying why patients with higher brown fat activity often display better insulin sensitivity. Together, these data give clinicians a practical toolbox for a therapy that is both physiologic and patient‑friendly.
The take‑home message is simple: brown‑fat activation isn’t a mystical shortcut, it’s a modest, evidence‑driven lever you can pull with everyday habits. By layering a brief, tolerable cold stimulus, a cup of catechin‑rich tea, and, when appropriate, a low‑dose capsaicin supplement, most healthy adults can safely nudge their energy balance toward a slightly higher baseline. As we continue to refine imaging biomarkers and explore gene‑editing frontiers, the real excitement lies in empowering each of us to claim your metabolic edge—not through fad diets or miracle pills, but through a handful of science‑backed tweaks that fit neatly into a busy life. Stay curious, stay measured, and let your own brown fat do some of the work.
Frequently Asked Questions
How long and how cold should a typical “cold exposure” session be to reliably stimulate brown fat without risking hypothermia?
I usually tell patients that a “cold‑exposure” session doesn’t have to feel like an Antarctic plunge. Aim for 10‑20 minutes at a comfortably chilly room temperature—about 14‑19 °C (57‑66 °F)—or, if you’re feeling adventurous, a brief 2‑5‑minute dip in water that’s 4‑10 °C (39‑50 °F). Do this 3‑4 times a week, stay clothed enough to avoid shivering, and stop if you start to feel numb or dizzy. That’s enough to nudge brown‑fat activity without courting hypothermia.
Which dietary supplements have the strongest clinical evidence for enhancing brown adipose tissue activity, and are there any safety concerns?
Based on limited human trials, only a few supplements consistently nudge brown‑fat activity: modest doses of capsaicin (or capsinoids), mirabegron (a β3‑adrenergic agonist approved for overactive bladder), and high‑dose omega‑3 EPA/DHA with a low‑carb, high‑protein diet. Capsaicin raises BAT glucose uptake ~10‑15% but can cause GI irritation >4 mg/day. Mirabegron may increase heart rate and blood pressure, so it’s off‑label. Omega‑3s are generally safe, though excess may affect bleeding. Discuss with your clinician before starting.
Can imaging techniques like PET‑CT or infrared thermography be used in a primary‑care setting to confirm that a patient’s brown fat is actually responding to a given protocol?
I’m often asked whether we can “see” brown‑fat kicking in right at the clinic. In theory, a fluorodeoxyglucose PET‑CT is the gold‑standard for visualising active brown adipose tissue, but the scan is expensive, involves ionising radiation and requires a nuclear‑medicine specialist to interpret the images—so it’s not a realistic primary‑care tool. Infrared thermography is cheaper and radiation‑free, yet its resolution is too coarse and there’s limited validation for tracking protocol‑driven activation. In practice, we usually rely on indirect markers (e.g., changes in resting metabolic rate or glucose tolerance) and refer patients for imaging only when a research or specialist evaluation is warranted.




